Table of Contents
Is It Hypoxemia or Hypoxia? Know the Life and Law Difference in Florida
Hypoxemia means your arterial blood oxygen drops below normal, while hypoxia means your organs starve for oxygen, even if blood levels look adequate. Cleveland Clinic clarifies that hypoxemia can lead to hypoxia but the two do not always overlap. A peer reviewed MD Anderson briefing underscores that you may be hypoxic without measurable hypoxemia when flow or hemoglobin is impaired. Johns Hopkins notes that birth asphyxia first triggers hypoxemia, then tissue hypoxia and acidosis in newborns. Recognizing which problem occurred and when allows Percy Martinez to pinpoint the exact moment a Florida provider breached the standard of care, turning a medical crisis into an actionable malpractice claim.
Warning Signs Hospitals Miss and When That Lapse Equals Malpractice
Florida ICUs and delivery rooms deploy pulse oximeters, arterial blood gas checks, and ventilator alarms, yet staff still overlook falling saturations or silence beeps. Bounds Law’s review of litigation shows defendants often blame equipment malfunction, but courts hold teams liable for failing to confirm accuracy and intervene quickly. We cannot stress enough how hypoxia can exist despite “acceptable” SpO₂ if perfusion is poor, meaning clinicians must correlate vitals with patient color and mentation, not numbers alone. When nurses ignore a drop below 90 percent or delay supplemental oxygen, tissue damage begins within minutes, and Percy’s experts translate each missed reading into a clear timeline of negligence that resonates with juries statewide.
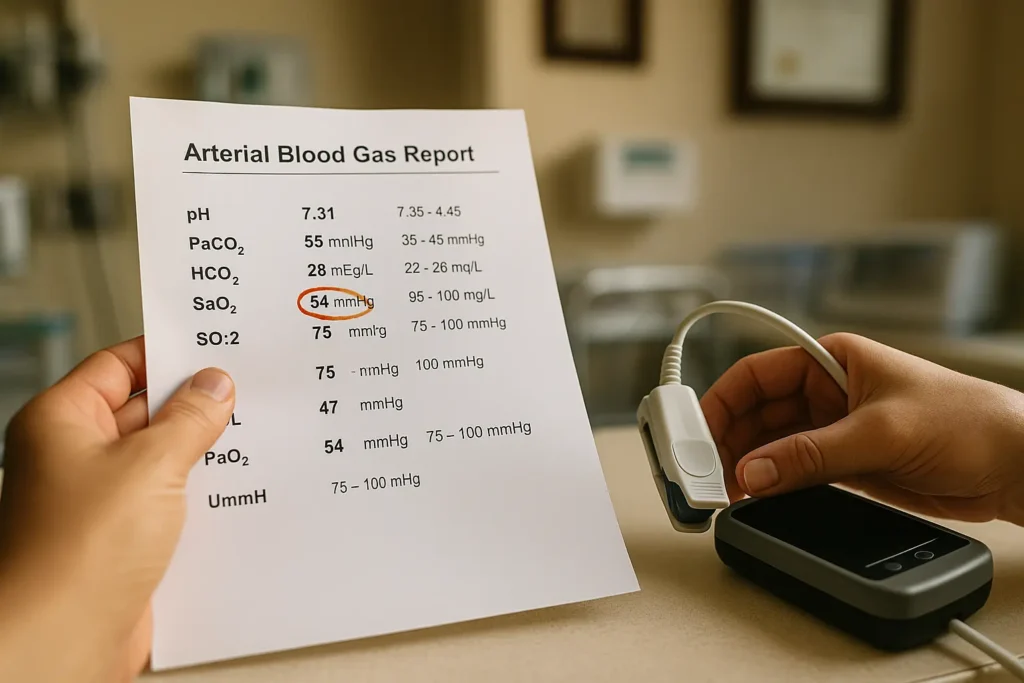
The Paper and Pixel Trail Percy Captures Within 48 Hours
Under §766.106, Florida plaintiffs must support claims with verified medical records and a corroborating expert affidavit before filing suit. Percy’s team issues HIPAA compliant requests the same day you call, then audits pulse ox waveforms, ventilator logs, and nursing notes for post event edits, often revealing hidden periods of hypoxia that chart summaries omit. Anidjar & Levine notes that proving hypoxic brain injury hinges on linking these records to an expert opinion that the provider deviated from the standard of care. Our proprietary O₂ Forensics™ software overlays time stamped vitals with medication pushes, building a persuasive visual that insurers cannot ignore.
Beat the Clock: Statutes, Presuit Notices, and Oxygen Case Deadlines
You generally have two years from when negligence is discovered and no more than four years from the event to sue in Florida, with a special extension to a child’s eighth birthday for birth injuries. Before filing, §766 demands a 90 day presuit notice and expert review, during which hospitals may “investigate” and even destroy electronic logs after 30 days unless legally preserved. Percy Martinez triggers litigation hold letters within 24 hours and, if needed, seeks emergency injunctions in Miami Dade, Hillsborough, or Orange County courts to freeze NICU servers, stopping data loss before it sabotages your claim.
Transparent Payouts: What Hypoxia Settlements Really Look Like
Recent public verdicts show a $2.5 million settlement for neonatal HIE in Florida and an average U.S. malpractice payout near $329k, with birth related hypoxia cases topping seven figures. These numbers rise when lifelong oxygen therapy, seizure control, or cerebral palsy care is required. Percy’s finance experts separate taxable and non taxable portions, ensuring “clean revenue” that passes lien audits and keeps future Medicaid benefits intact, crucial for families budgeting decades of therapy.
Why Top Hospitals Respect and Defendants Fear Percy Martinez
With thirty years of trial wins and a 98 percent pre trial settlement rate, Percy Martinez has secured record recoveries for hypoxia victims from Miami to Pensacola. Families choose us because we absorb all case costs, provide bilingual updates, and leverage verdict data hospitals recognize. Florida malpractice analysts cite Percy’s neonatal encephalopathy wins in Orlando and Tampa as benchmarks other firms cite in their marketing. Our courtroom demonstratives, animated oxygen deprivation timelines synced to infant heart rate tracings, turn complex physiology into vivid storytelling that juries remember.

Act Before Data Disappears: Book Your Free Oxygen Injury Audit Now
Call (305) 529-0001 or upload your records through our encrypted portal today. Percy’s team will confirm within two business hours, dispatch record requests within one day, and appear in any Florida county court within 48 hours if emergency preservation is needed. Because neonatal ventilator logs overwrite after 30 days and adult ICU monitors cycle data even faster, every hour counts. Your consultation is free, we front all costs, and you pay nothing unless we win, so your path from crisis to compensation starts with a single click.




